Gastroesophageal reflux disease
from symptoms to treatment
What should I know about the esophagus?
The esophagus is the part of the digestive tube that connects the pharynx to the stomach and whose role is to propel food downwards.
It is approximately two centimeters in diameter and 20 cm long.
The lining of the esophagus consists in four layers. The innermost layer, the mucosa, is made up of several types of cell that constitute the squamous epithelium, a lining tissue. At either end of the esophagus there is a sphincter – a bundle of muscles that control the descent of food and prevent it from coming back up.
What are the symptoms of GERD?
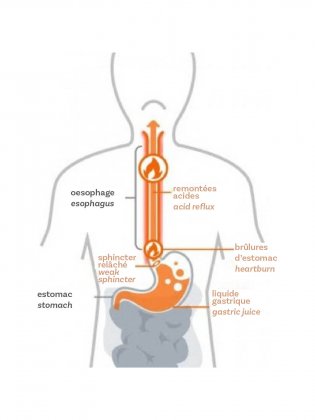
GERD occurs when acid flows from the stomach back up into the esophagus, sometimes travelling all the way to the mouth, because of a problem affecting the lower esophagus sphincter (LES).
The most frequent symptom is heartburn, also known as pyrosis, a burning sensation that starts behind the sternum and moves upward. It generally occurs after meals or when the person bends forward or lies down.
Other less typical but very frequent symptoms include:
- Chronic, unexplained cough
- Chest pain
- Epigastric pain
- ENT symptoms such as laryngitis, pharyngitis or burning sensations
- Sensation of having a lump in the throat
If symptoms persist, seek medical assistance. The mucosa of the esophagus is not designed to tolerate acidity.
What are the risk factors for GERD?
Several factors can lead to gastroesophageal reflux:
- Hiatal hernia (when the stomach moves up through the hiatus, a small opening in the diaphragm)
- Certain medications including progesterone, acetylsalicylic acid (aspirin) and non-steroidal anti-inflammatory drugs (NSAIDs)
- Excessive pressure on the abdomen caused by excess weight, obesity or pregnancy
- Lifestyle and dietary factors: stress; smoking; consumption of alcohol, chocolate, spices, acidic or fatty foods; a large meal before bed
How is GERD diagnosed?
GERD is often diagnosed using empirical reasoning based on the patient’s medical history and the specific nature of signs such as heartburn and acid regurgitation.
Additional exploratory exams are useful if medical treatment fails or in the case of a preoperative check-up or diagnostic uncertainty (atypical symptoms).
An endoscopy of the esophagus, stomach and duodenum (esophagogastroduodenoscopy, or EGD) is the leading exam to explore atypical symptoms and/or for patients aged 50 and older. It is used to diagnose GERD when the following lesions occur:
- Barrett’s esophagus, a precancerous condition in which the squamous epithelium changes to intestinal epithelium
- Peptic esophagitis, characterized by inflammation that damages the mucosa
When the endoscopy results are normal, pH testing is indicated. A small probe or a capsule attached to the esophagus wall measures acid reflux for 48 to 96 hours.
What are the treatment options for GERD?
- Lifestyle and dietary recommendations:
- Avoid overly large meals with high quantities of fatty foods
- Avoid lying down too soon after eating, especially at bedtime. If possible, wait at least two hours after a meal, and raise the head of your bed by a few inches.
- Lose excess abdominal weight
- Avoid identified triggering foods such as white wine, spices, chocolate, alcohol, tea, citrus juices and fatty foods, as well as smoking.
- Antacids, alginates and H2 blockers reduce acid secretions and relieve symptoms.
- Proton pump inhibitors (PPIs) taken 15 to 20 minutes before mealtime greatly reduce the amount of acid secreted by the stomach.
- Surgery is rarely indicated but may be appropriate for young patients in good physical health who take PPIs on a daily basis to treat GERD complicated by esophageal stricture (narrowing of the lower part of the esophagus) or a large hiatal hernia.
The main surgery is fundoplication (Nissen or Toupet fundoplication), which consists in winding the top of the stomach around the lower part of the esophagus. This reduces the size of the hiatus and strengthens the valve between the esophagus and the lower esophageal sphincter, thus diminishing the acid reflux.
- Promising new endoscopic techniques are currently being developed to treat GERD.
Chiffres clés
-
5 to 10 percent of adults suffer from GERD on a daily basis
-
20 to 30 percent of endoscopic exams reveal the presence of peptic esophagitis
-
30 to 40 percent of adults occasionally experience heartburn and/or regurgitation
-
IPPs relieve symptoms in approximately 70 percent of cases
