Breast Radiology
Leading-edge technology dedicated to latest-generation imaging
Leading-edge technology
The American Hospital of Paris is equipped with one of the ten most advanced mammography systems in the world. Digital breast tomosynthesis (3D imaging method) offers better viewing, which in turn leads to more accurate diagnoses. All supplementary exams can be performed on site on very short notice, including MRI, microbiopsy and macrobiopsy testing.
3D MAMMOGRAPHY
One of the most important technological advances in recent years is breast tomosynthesis.
This 3D mammography technique consists in moving the x-ray tube around the breast to capture multiple images at the same time, as opposed to a single image captured with traditional mammography.
The images are reconstructed, or synthesized, using an algorithm similar to the one used by a CT scan. This technology facilitates the detection of early-stage cancer in a normal mammary gland, and makes it easier to distinguish dense, fibrous breast tissue which could lead to a false-positive.
A large study involving 200,000 women showed a nearly 30 percent relative increase in the number of cancers detected using this technique.
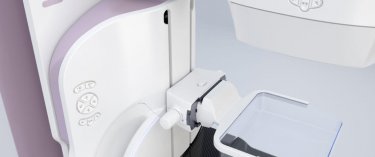
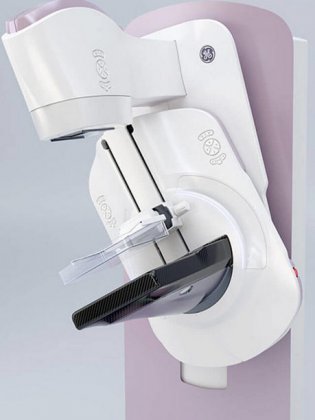
The American Hospital of Paris has acquired a new latest-generation 3D mammography device. Its rounded angles and reassuring design in pastel pink and white tones help to create a more user-friendly and less stressful experience for patients. The device’s technical features are also as discrete as possible, eliminating an additional stress factor for women.
With this system, the technician begins compressing the breast as usual, then gives the patient a remote control device which she can then use (if she wishes) to continue compressing her breast. This enables her to play an active role in the exam while improving her tolerance for this step of the procedure.
Our new breast tomosynthesis device is part of our comprehensive approach to personalized patient care, provided by dedicated radiologists and technicians.
BREAST ULTRASOUND
This pain-free exam, which uses high frequency sound waves instead of x-rays, is performed at the discretion of the radiologist after a screening mammogram.
It is particularly recommended when dense breasts are revealed by the mammogram, or to investigate or rule out an abnormality detected on the mammogram.
At the American Hospital of Paris, we use a latest-generation ultrasound device exclusively dedicated to breast exams. Because the images are produced approximately 200 times faster than with conventional ultrasound systems, they are exceptionally high-quality, homogenous, high-definition and informative.
We also use elastography to view and analyze tissue “stiffness” in real time. Tissue stiffness has become a very important parameter in ultrasound imaging for the diagnosis of potentially malignant lesions.
This parameter is now used in international classifications of breast abnormalities and is said to help reduce the number of unnecessary biopsies.
Breast MRI
This exam takes about fifteen minutes and requires no radiation. Instead, an iodinated contrast agent, well-tolerated by patients, is injected.
MRI is the gold standard for detecting breast cancer in very high-risk patients (those with an inherited gene mutation or who underwent chest radiation for hematologic disease between the ages of 10 and 30).
This exam is also indicated for women diagnosed with breast cancer before the age of 40, to assess certain types of breast cancer or in the case of specific treatments such as preoperative chemotherapy. Lastly, it can be used to determine whether a breast implant has ruptured.
MRI will probably play an increasingly crucial role in indications that are currently still under debate, such as pre-operative assessments for non-locally advanced breast cancers. Some recent studies have shown that the rate of revision surgery (when a second surgical procedure is necessary) was divided in half in patients having undergone a systematic preoperative MRI.
When breast cancer is discovered in a patient with high mammographic breast density, which can “mask” a cancerous lesion, an MRI might also be performed to search for other abnormalities that cannot be detected with a mammogram.
Unless it is being employed as part of the proven strategy of regularly monitoring very high-risk patients (with an identified genetic risk), an MRI is often performed as a second-line exam whose results must be analyzed in combination with all other exams performed.
INTERVENTIONAL SENOLOGY
It includes all practices aimed at establishing a histological diagnosis (under the microscope) or preparing the surgeon's operation in case of an intervention.
Thanks to our increasingly sophisticated equipment, we are able to detect lesions that are increasingly small and cannot be felt by the patient or her doctor.
To analyze them, we use sampling techniques (cytoponctions, microbiopsies and macrobiopsies). These procedures are guided by ultrasound, mammography and sometimes even MRI.
Cytopunctions with a fine needle are reserved for the study of lymph nodes or for the evacuation of a troublesome or painful cyst.
Microbiopsies are used in ultrasound to analyze a mass. The patient lies on the ultrasound table and after disinfection and local anesthesia, the sample is taken and sent to the laboratory for microscopic analysis.
Macrobiopsies can be used for ultrasound, mammography or MRI. They are most often used with mammographic guidance to analyze microcalcifications discovered in mammography. With our new system, the patient is in a sitting, lying or semi-lying position, the breast is compressed, centered on the area of calcifications and after disinfection and local anesthesia, the samples are taken automatically with a dedicated latest generation device. Today, it is also possible to perform biopsies under 3D tomosynthesis. After these samples are taken, a clip (a small titanium marker) is left in place to be used for preoperative identification in case of surgical indication. If the lesion is benign, thanks to this technique under local anaesthesia, on an outpatient basis and without hospitalization, the patient will have avoided a surgical procedure.
The purpose of the preoperative location is to help the surgeon to remove a non palpable lesion. The procedure is usually performed within 24 hours before surgery, by inserting a guide wire into the breast, after disinfection and local anesthesia, in the center of the lesion, using mammography (microcalcifications) or ultrasound (mass) as a guide.
RETOUR VERS LA PAGE DU BREAST CENTER


